
(Photo by Edward Jenner via Pexels)
By Stephen Beech
Tiny sensors could soon be able to "sniff" bodily fluids to diagnose bacterial infections and detect antimicrobial resistance.
The minuscule devices would operate similarly to breathalyzers, according to scientists.
They say developing the technology could provide "affordable and rapid" diagnostic tests, which would improve treatment plans and help combat antibiotic resistance.
A team of engineers, microbiologists, and machine learning experts made the claims in the journal Cell Biomaterials.
Senior author Professor Andreas Güntner, a mechanical and process engineer at the Swiss university ETH Zurich, said: “One of the biggest drivers of antimicrobial resistance is that we lack rapid diagnostics.
“Our idea is to bypass laboratory analysis, which is a multi-step process that usually takes hours to days - and sometimes even weeks - with a simple test that gives results within seconds to minutes.”

(Photo by Edward Jenner via Pexels)
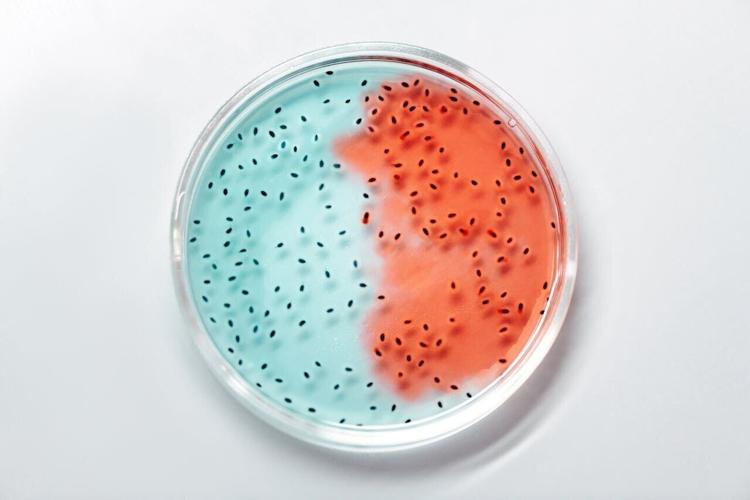
Doctors have traditionally used their noses to diagnose bacterial infections. For example, Pseudomonas aeruginosa infections exude a sweet, grape-like scent, whereas Clostridium infections have a foul, putrid smell.
The odors are due to the presence of volatile organic compounds (VOCs) - tiny molecules emitted by microbes and other organisms that often carry distinctive smells.
Instead of using our noses, the researchers propose developing chemical sensors to detect bacteria-associated VOCs in bodily fluids, including blood, urine and phlegm.
Similar technologies are used to detect specific molecules in alcohol breathalyzers and air-quality monitoring devices.
Güntner said: “We have already developed and commercialized something similar for detecting contaminations like methanol in alcoholic beverages.
“Now, we are trying to transfer this technology to more complex situations.”

(Photo by Polina Tankilevitch via Pexels)
He says that, even within the same species, different strains of bacteria can emit different combinations or concentrations of VOCs.
The research team believes that means the sensors could be used to identify infections caused by antimicrobial-resistant bacteria.
The concept has already been demonstrated in lab conditions. A previous study showed that VOC signatures can differentiate methicillin-resistant Staphylococcus aureus (MRSA) from non-resistant strains.
However, developing sensors for use in clinical practice will require more research.
As the VOC concentrations emitted by bacteria are extremely low, Güntner described the development of suitable sensors is "challenging."
He said, “Imagine you have a room full of one billion tiny balls, and all of them are blue except for one red ball.
“To differentiate between different bacteria types, you must be able to recognise and distinguish that situation within seconds from a situation where three or four red balls are present.”
Because bacteria emit thousands of different VOCs, the researchers say the devices will need to include a combination of sensors with different binding capacities.

(Photo by Anna Tarazevich via Pexels)
The sensors could be made using materials including metal oxides, polymers, graphene derivatives, and carbon nanotubules and would be designed using recent advances in nano- and molecular-scale engineering.
To streamline detection, the devices would also need to be equipped with filters to remove compounds that are uninformative.
The researchers say that machine learning algorithms will play a "vital" role in guiding the sensor design.
Güntner said: “Machine learning will be essential for identifying the smallest combinations of VOCs that can distinguish different types of bacteria and give information on antimicrobial resistance and virulence."
But, once developed, the sensors would offer a quick, transportable method for diagnosing bacterial infections that could be used without significant training.
Güntner added: “The overall goal is to translate scientific advances in VOC analysis into practical, reliable tools that can be used in everyday medical practice.
“Ultimately, we hope this will improve patient outcomes and support antibiotic stewardship.”












(0) comments
Welcome to the discussion.
Log In
Keep it Clean. Please avoid obscene, vulgar, lewd, racist or sexually-oriented language.
PLEASE TURN OFF YOUR CAPS LOCK.
Don't Threaten. Threats of harming another person will not be tolerated.
Be Truthful. Don't knowingly lie about anyone or anything.
Be Nice. No racism, sexism or any sort of -ism that is degrading to another person.
Be Proactive. Use the 'Report' link on each comment to let us know of abusive posts.
Share with Us. We'd love to hear eyewitness accounts, the history behind an article.