
Geoffroy Laumet, MSU Associate Professor of Physiology, and Sabrina De Souza, MSU postdoctoral researcher, review a sample in Laumet's lab. (Finn Gomez, MSU College of Natural Science via SWNS)
By Stephen Beech
Chronic pain really does last longer for women than men - and it may be down to hormones, suggests a new study.
Hormone-regulated cells play a "key" role in resolving pain, according to the findings.
American scientists discovered that a group of white blood cells called monocytes release a molecule to switch off pain.
They found that the cells are more active in males due to higher levels of sex hormones, such as testosterone.
But females experienced longer-lasting pain and delayed recovery, because their monocytes were less active.
The researchers discovered the same pattern in both mice and human patients.
They say their findings, published in the journal Science Immunology, could mean those immune cells can be manipulated into producing more signals to calm pain.
While a new treatment is likely decades away, the team hope their research could one day help millions of people experience relief through non-opioid treatments - and ensure women’s pain is taken seriously.
Study co-author Professor Geoffroy Laumet said: “The difference in pain between men and women has a biological basis.

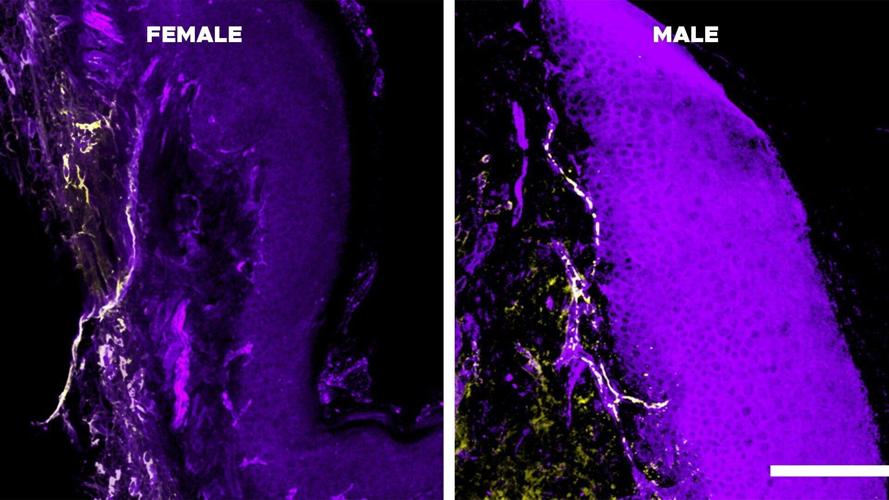
These side-by-side microscope images demonstrate lower IL-10 receptor subunit levels, shown in yellow, in female skin cells (left) than in male cells (right). (Laumet lab via SWNS)
“It’s not in your head, and you’re not soft. It’s in your immune system.”
He explained that pain results when neurons found throughout your body are activated by stimulation.
Most of the time they’re silent, but they become activated when people stub a toe or fall off a bike.
But for those with chronic pain, the sensors may be activated through mild stimulation, or even no stimulation at all.
Doctors still rely on patients rating their pain on a scale of one to 10.
But previous research has shown the problem is everyone experiences pain differently.
So, when more women than men complain of long-lasting or chronic pain, the difference is often put down to perception or reporting.
Laumet has devoted his lab at Michigan State University to studying pain for six years.

(Photo by kaboompics via Pexels)
His team was researching a small pilot project when they noticed higher levels of interleukin-10, or IL-10, in males.
When the second test again showed higher levels of the substance that signals to neurons to shut down pain, they realised they were onto something.
Study co-author Jaewon Sim, a former graduate student in Laumet's lab, said: “That was the turning point for me."
She added: “I feel extremely fortunate that we trusted those early, uncertain findings and chose to pursue them further.”
Laumet’s team employed a sophisticated technique called high-dimensional spectral flow cytometry.
They learned that monocytes, long thought to be precursor cells without much of a function, play an "essential and direct" role in communicating with pain-sensing neurons by producing IL-10.
The researchers found that IL-10-producing-monocytes were much more active in males than females.
When they blocked male sex hormones, they received the opposite result.

Aaryn Edwards, MSU graduate student, and Geoffroy Laumet, MSU Associate Professor of Physiology, work on a sample in Laumet's lab. (Finn Gomez, MSU College of Natural Science via SWNS)
Laumet said: “This study shows that pain resolution is not a passive process.
“It is an active, immune-driven one.”
The researchers performed at least five types of tests on mice to make sure what they saw wasn’t an anomaly.
Each time, the results were the same.
Laumet then contacted Dr. Sarah Linnstaedt at the University of North Carolina at Chapel Hill who was studying the psychological outcomes of people in car accidents.
Her research showed a similar pattern - men had more active IL-10-producing-monocytes and resolved pain faster.
Laumet says the new evidence illuminates the immune–neural pain resolution pathway, shifting the thinking from how pain starts to why pain persists.
He said the next step is to investigate how treatments could target that pathway and boost IL-10 production.
Laumet says such treatments could help pain resolve faster instead of just blocking pain signals.
He added: “Future researchers can build on this work.
“This opens new avenues for non-opioid therapies aimed at preventing chronic pain before it’s established.”




















(0) comments
Welcome to the discussion.
Log In
Keep it Clean. Please avoid obscene, vulgar, lewd, racist or sexually-oriented language.
PLEASE TURN OFF YOUR CAPS LOCK.
Don't Threaten. Threats of harming another person will not be tolerated.
Be Truthful. Don't knowingly lie about anyone or anything.
Be Nice. No racism, sexism or any sort of -ism that is degrading to another person.
Be Proactive. Use the 'Report' link on each comment to let us know of abusive posts.
Share with Us. We'd love to hear eyewitness accounts, the history behind an article.